Blog
Protecting the Periwound
Practical Techniques to Reduce Skin Breakdown
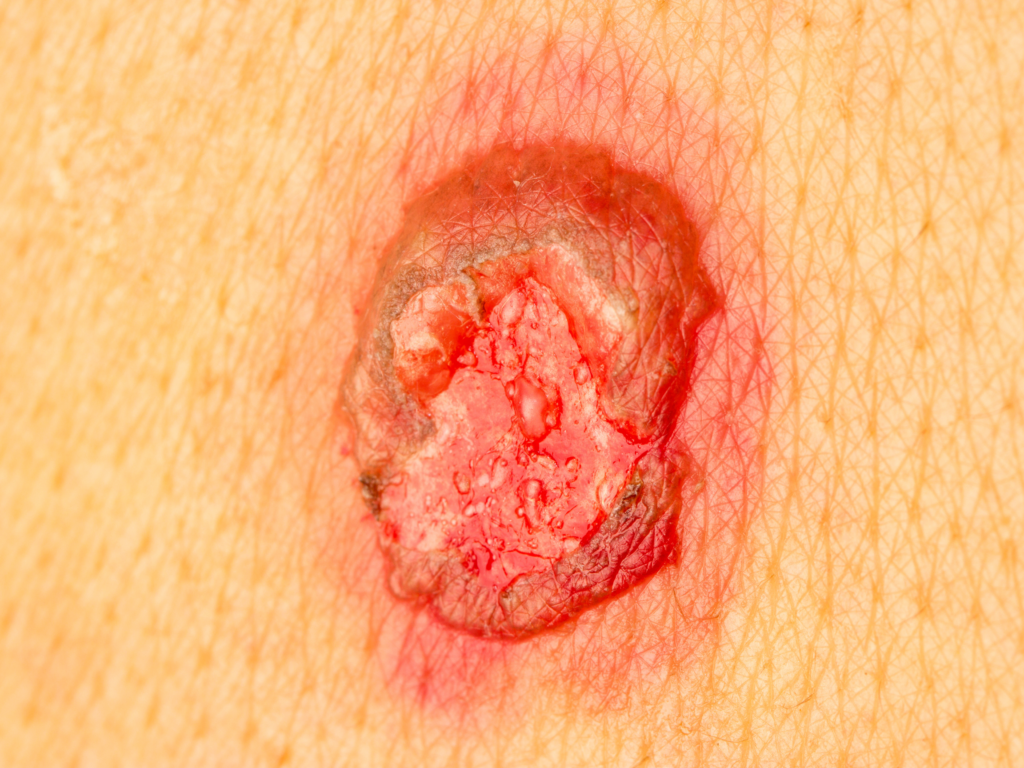
The periwound—the 4–6 cm of skin surrounding a wound—is essential for maintaining moisture balance, providing barrier protection, and ensuring dressing adhesion. Yet studies show that up to 80% of chronic wounds develop measurable periwound irritation or maceration at some point during treatment (Wounds International, 2022). When this skin breaks down, clinicians face higher infection risks, delayed epithelialization, dressing failure, and increased patient discomfort.
This guide outlines the causes of periwound damage, how to assess early warning signs, step-by-step protection techniques, and the latest best practices for safeguarding dressing edges.
Why the Periwound Matters in Every Dressing Change
Healthy periwound tissue directly influences the wound’s ability to progress through healing. Research published in Journal of Wound Care (2023) found that periwound compromise can delay healing by 50% or more due to moisture imbalance, dressing disruption, and increased inflammation.
When the periwound deteriorates, clinicians often see:
- Exudate leakage
- Dressing adherence issues
- Increased pain
- Maceration or denudement
- Higher infection probability
- Prolonged treatment time
Recent reviews continue reinforcing the same message: preserving skin integrity is a cornerstone of modern wound management.
1. Common Causes of Periwound Breakdown
Moisture and Exudate Overload (Maceration)
Maceration affects nearly 70% of chronic wounds (Wounds UK, 2022). Prolonged moisture contact causes the skin to appear pale, boggy, and fragile—conditions that increase the likelihood of breakdown and cause adhesives to fail.
A new 2025 review highlights that exudate overload significantly weakens adjacent periwound barrier function, adding measurable risk to both tissue integrity and dressing stability (Mervis et al., 2025).
Adhesive Trauma (MARSI)
Medical adhesive–related skin injury affects 15–20% of hospitalized patients and is more common in those with fragile or aging skin (MARSI Consensus Panel, 2020).
Infection and Inflammation Spread
Up to 60% of chronic wounds contain biofilm, which can extend into periwound tissue when unmanaged (EWMA, 2023). This presents as erythema, warmth, tenderness, or swelling.
Shear and Friction
Movement, repositioning, and rolling dressing edges create shear forces that compromise the skin. High-mobility anatomical sites are particularly at risk.
Chemical Irritation
Urine, stool, harsh cleansers, or incompatible topical agents can cause dermatitis and weaken superficial tissue.
2. How to Assess Early Warning Signs
Periwound assessment should occur at every dressing change. Watch closely for:
- Color changes (persistent redness, blanching, pallor)
- Texture changes (boggy, overly dry, flaky, or waterlogged skin)
- Pain or tenderness (especially new onset)
- Adhesive imprints (stripping, skin tears, shiny patches)
- Edema or firmness
- Heat or odor indicating early infection
- Sudden increases in moisture around the dressing edge
A 2024 integrative review in Wound Practice & Research emphasizes that gentle cleansing with mild, non-alkaline, pH-balanced products supports skin resilience and reduces periwound irritation (O’Brien et al., 2024).
3. Step-by-Step Periwound Protection Techniques
Step 1: Use Gentle, Non-Cytotoxic Cleansers
Use sterile saline or a mild, pH-balanced cleanser. Avoid scrubbing. Pat dry.
Step 2: Manage Exudate Proactively
Exudate is one of the strongest predictors of periwound breakdown. Proper dressing selection and frequent reassessment are essential.
Recent 2025 evidence notes that silicone foam dressings can help maintain moisture balance and reduce periwound maceration in wounds with moderate-to-heavy exudate (Mervis et al., 2025). Maintaining an airtight seal prevents pooling toward the periwound.
Step 3: Apply Barrier Film or Protectant Layer
Barrier films reduce MARSI incidence by nearly 27% (Journal of Wound Care, 2023). Apply uniformly and allow it to dry before the dressing is placed.
Step 4: Add Protective Cushioning if Needed
Use silicone interfaces or foam layers in high-friction zones to minimize shear.
Step 5: Reduce Adhesive Trauma
Silicone adhesives significantly reduce stripping compared to acrylic. Remove dressings slowly, supporting the skin as you lift.
Step 6: Fit Dressings Correctly for a Secure Seal
A properly sized dressing or NPWT drape protects against leaks, shear, and moisture exposure.
4. Best Practices for Protecting Dressing Edges
Dressing edges are one of the most common sources of periwound failure.
To protect this vulnerable interface:
- Smooth all edges to prevent rolling
- Avoid stretching adhesives during placement
- Add supplemental silicone tape for high-motion areas
- Trim any lifted sections early
- Monitor seal integrity frequently—especially with NPWT
Rotate adhesive placement when possible to reduce repeated trauma
Protecting the Periwound Protects Outcomes
Periwound protection is a proactive strategy—and one of the most cost-effective ways to support healing. With early assessment, moisture control, gentle cleansing, and smart dressing-edge management, clinicians can significantly reduce preventable complications.
References
- Wounds International. Best Practice for Maintaining Skin Integrity in Wound Care. 2022.
- Wounds UK. Maceration in Chronic Wounds: Clinical Challenges. 2022.
- Journal of Wound Care. Impact of Periwound Health on Healing Duration. 2023.
- MARSI Consensus Panel. Medical Adhesive–Related Skin Injury Guidelines. 2020.
- European Wound Management Association (EWMA). Biofilm in Chronic Wounds. 2023.
- O’Brien, A. et al. “What is the evidence on skin care for maintaining skin integrity and prevention of wounds?” Wound Practice & Research. 2024.
- Mervis, J. et al. “Impact of Chronic Wound Exudate on the Patient Journey and the Role of a Silicone Foam Dressing.” International Wound Journal. 2025.